Eleven years ago on February 2, 2012, Morton Plant Hospital in Clearwater, Florida became the first hospital in the Tampa Bay area to replace a heart valve without open heart surgery. The structural heart team, led by Joshua Rovin, MD, FACS, cardiovascular surgeon and medical director of The Center for Advanced Valve and Structural Heart Care at Morton Plant Hospital, performed what was then a new procedure, Transcatheter Aortic Valve Replacement or TAVR.
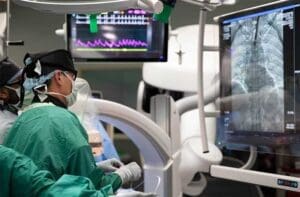 TAVR is a minimally invasive heart valve replacement surgery used to treat severe aortic stenosis, or narrowing of the aortic valve, which increases the workload and strain on the heart. Instead of opening the chest, doctors insert a catheter into an artery, usually in the groin area, and guide it into the heart, implanting a new aortic heart valve inside the original diseased valve.
TAVR is a minimally invasive heart valve replacement surgery used to treat severe aortic stenosis, or narrowing of the aortic valve, which increases the workload and strain on the heart. Instead of opening the chest, doctors insert a catheter into an artery, usually in the groin area, and guide it into the heart, implanting a new aortic heart valve inside the original diseased valve.
History of the Program
Though the first TAVR procedure was done in 2012, the vision started years earlier in 2008 when Dr. Rovin joined John Ofenloch, MD, cardiovascular surgeon, and chief of Cardiovascular and Thoracic Surgery at MPH. The two shared their vision for a multidisciplinary heart team and an Advanced Valve and Structural Heart Center at Morton Plant with then hospital president, Kris Hoce, and cardiology leaders.
Hoce grasped their vision and collaborated with the surgeons, building a facility to perform the surgery and developing an experienced team to accomplish their goal. One of the rooms from the original Morgan Heart Hospital project had been left empty as a shell for future growth. By December 2011, with funding from the Morton Plant Mease HealthCare Foundation, that shell was transformed into a hybrid operating room, the first of its kind in the Tampa Bay region. A hybrid operating room can provide advanced imaging for complex cardiovascular surgery requiring x-ray (fluoroscopic imaging), including TAVR.
Multidisciplinary Team
While the hybrid suite was being constructed, Drs. Ofenloch and Rovin assembled a heart team. After collaborating with other cardiovascular leaders across the country, they knew the best patient outcomes would be delivered by a multidisciplinary team of cardiovascular professionals.
“We wanted passionate physicians who were team players,” Dr. Rovin said. “To bring significant contributions to the team, people had to be willing to set aside their own agendas and egos.”
The original team included interventional cardiologists Lang Lin, MD, and Douglas Spriggs, MD; noninvasive cardiologists Mike Barry, MD, and Todd Kovach, MD, as well as Drs. Rovin and Ofenloch.
“We were very lucky to bring that amazing group of people together,” Dr. Ofenloch said. “It was uncommon to have a multidisciplinary team of cardiovascular experts outside of an academic setting, but this was one component that made our program unique.”
The team now includes cardiothoracic surgeon Michael Kayatta, MD; noninvasive cardiologists Wayne Cheng, MD, and Jorge Navas, MD; interventional cardiologist Ravi Kethireddy, MD, and original team members Drs. Barry, Kovach, Lin, Rovin and Ofenloch. Advanced practical registered nurses Lisa Stone, Mamata Pandya and Jennifer Deering-Darza are also part of this team that meets weekly to discuss every patient, review cardiac imaging and determine the best course of treatment. The meetings provide opportunities for input from doctors with different areas of expertise to share and debate possibilities, ensuring nothing is overlooked and a customized treatment plan is created for each patient.
Program’s Growth
The first year the team performed 50 cases, but many other patients who were screened were not even candidates due to severe illness or advanced age. “The delivery devices were very large and often unsuitable for many patients,” Dr. Rovin said.
The heart valve industry recognized the high-quality outcomes and large volume of cases performed at Morton Plant and invited the team to participate in several national clinical trials. The trials gave Morton Plant access to the latest and most advanced devices, which meant smaller delivery systems that would work for a larger number of patients. The hospital’s involvement in the clinical trials gave the community access to the latest cutting-edge treatments for patients with aortic stenosis.
“We were fortunate from almost the beginning to have access to so many trials. Research is vital to bring high quality health care to our community,” Dr. Rovin said.
Grateful Patient
Opportunities to participate in clinical trials have been game changers for many patients including Vera Nigrelli. She would have undergone open heart surgery if the TAVR option had not come through.
When she was 75, her cardiologist told her she had severe stenosis. She knew she needed something done. “I couldn’t walk far or fast, but I was scared to have open heart surgery,” she said.
A week before she was scheduled to undergo open heart surgery, she received a call informing her she had been approved to participate in a clinical trial.
“My TAVR surgery couldn’t have been easier, and I couldn’t be happier,” she said. “I had the surgery on a Tuesday, and on Friday, I went out to dinner.”
Four months later she was back at her Silver Sneakers class.
“I recently had an angioplasty and was told my veins are good and my heart is good,” added Nigrelli, who is now 82.
Nigrelli’s testimony could be repeated hundreds of times by patients who have been given renewed life as a result of TAVR.
“Over the past decade, we have seen so many patients and families express immense gratitude for the way TAVR has changed their lives,” said Dr Lin. “As physicians, our goal is to never take that for granted. We continually improve our knowledge and skills to always offer our patients the best treatment options.”
For more information, check out Morton Plant’s structural heart program.
BayCare’s Other Structural Heart Programs
The Valve Clinic at St. Joseph’s Heart and Vascular Institute in Tampa opened in 2014. The cardiovascular professionals at St. Joseph’s built an award-winning program with high volume to meet the needs of the community. Both Morton Plant and St. Joseph’s hospitals’ structural heart programs received the Transcatheter Valve Certification from the American College of Cardiology in 2022.
The Structural Heart and Valve Program at Winter Haven Hospital’s Bostick Heart Center started in 2020 with the strong support of experts from Morton Plant and the investment of BayCare. Having the knowledge and resources of BayCare’s other programs has allowed Winter Haven’s program to offer the highest quality cardiac care to the Winter Haven community.
BayCare’s structural heart programs also treat pulmonary stenosis, mitral stenosis, aortic regurgitation and mitral regurgitation. Depending on the severity of disease and other factors, patient treatment options may include medical management, minimally invasive valve repair, minimally invasive valve replacement or open-heart surgery.


